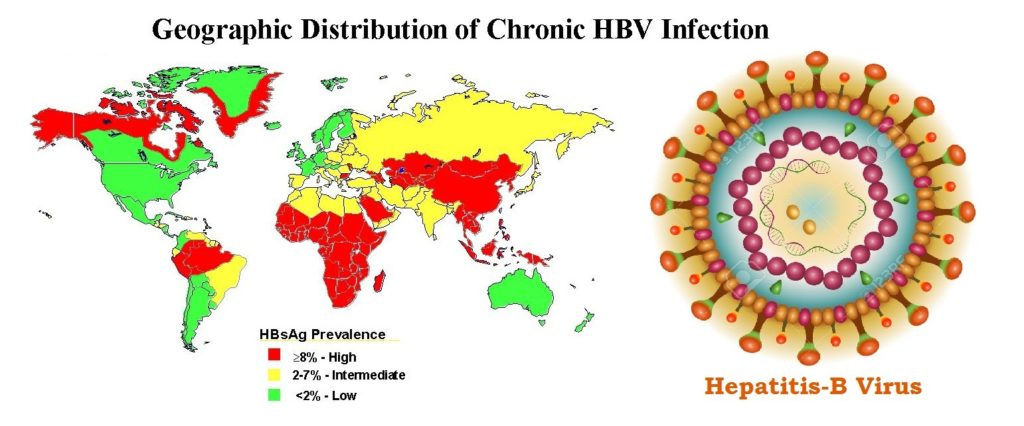
Incidence of mother-to-child transmission of hepatitis b in relation to maternal peripartum antiviral prophylaxis: A systematic review and meta-analysis. Yao N, Fu S, Wu Y, Tian Z, Feng Y, Li J, et al. “Global, regional, and national burden of hepatitis B, 1990-2019: A systematic analysis for the Global Burden of Disease Study 2019.” The lancet. 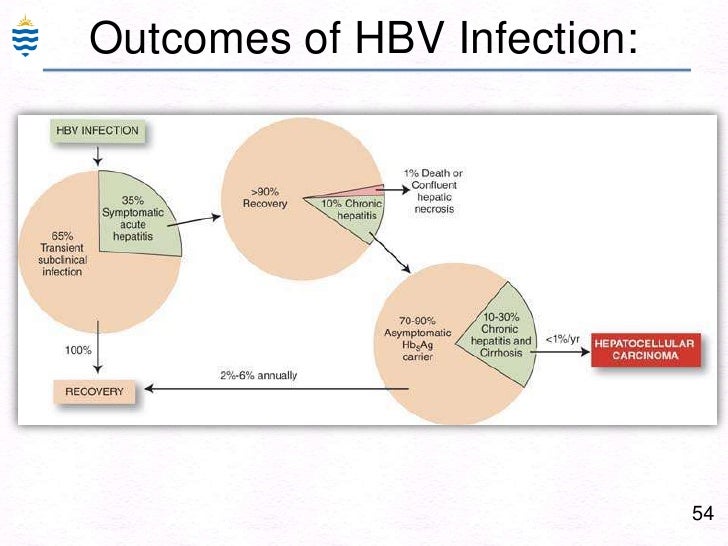 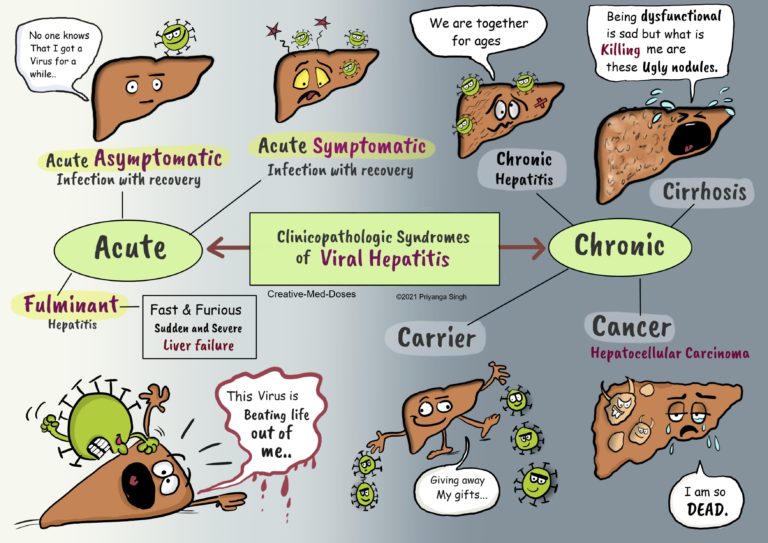
T-cell immunity effects hepatitis B virus immunological characteristics mother-to-child transmission pregnancy.Ĭopyright © 2023 Lu, Cao, Zhang, Yang, Bi, Lin, Deng, Jiang, Sun, Zeng, Lu, Zhang, Liu, Gao, Wu, Hao, Chen, Hu, Xu, Xiong, Dong, Song, Li and Xie. This article reviews the literature on immunological characteristics of chronic HBV-infected patients during pregnancy and postpartum, blocking mother-to-child transmissions and related immune mechanisms, hoping to provide new insights for the prevention of HBV MTCT and antiviral intervention during pregnancy and postpartum. Meanwhile, HBV humoral and T-cell responses are important for the durability of protection after fetal vaccination. The maternal and fetal T-cell immunity in HBV infection is important because adaptive immune responses, especially virus-specific CD8 T-cell responses, are largely responsible for viral clearance and disease pathogenesis during HBV infection. It is interesting to note that after delivery, the women who had a chronic HBV infection may spontaneously achieve HBeAg seroconversion and HBsAg seroclearance. The changes in the immune environment during pregnancy and the hepatotropic nature of HBV may be the main reasons for the adverse maternal outcomes. In addition, new research has indicated that HBV infection in the mother may also be linked to unfavorable outcomes such as gestational diabetes mellitus, intrahepatic cholestasis of pregnancy, and premature rupture of membranes. For example, IL-4 can mediate the beneficial effect on infants' HBsAb levels when maternal folic acid supplementation. Some studies have also found that some supplementation during pregnancy can increase cytokine levels and then affect the level of HBsAb in infants. Unfortunately, some infants still have chronic HBV infections. The passive-active immune program for children, which consists of the hepatitis B vaccine and hepatitis B immunoglobulin, and antiviral therapy for pregnant women who have a high HBV DNA load (greater than 2 × 10 5 IU/ml), are currently two of the most important ways to prevent the transmission of HBV from mother to child. HBV DNA high level, HBeAg positivity, placental barrier failure, and immaturity of the fetal immune are the possible causes of chronic HBV infection. Approximately 6.4 million children under the age of five have chronic HBV infections worldwide. One of the most common routes of chronic hepatitis B virus (HBV) infection is mother-to-child transmission (MTCT). 8 Department of Infectious Disease, Beijing Ditan Hospital, Capital Medical University, Beijing, China.7 Department of Infectious Disease, Haidian Hospital, Beijing Haidian Section of Peking University Third Hospital, Beijing, China.6 Department of General Surgery, Beijing Ditan Hospital, Capital Medical University, Beijing, China.5 Department of Hepatology Division 2, Peking University Ditan Teaching Hospital, Beijing, China.4 Infectious Disease Department, Xuanwu Hospital, Capital Medical University, Beijing, China. 
3 Department of Infectious Diseases, Miyun Teaching Hospital, Capital Medical University, Beijing, China.2 Department of Obstetrics and Gynecology, Wuhan Children's Hospital (Wuhan Maternal and Child Healthcare Hospital), Tongji Medical College, Huazhong University of Science and Technology, Wuhan, China.1 Department of Hepatology Division 2, Beijing Ditan Hospital, Capital Medical University, Beijing, China.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
